Shoulder arthritis is a widespread chronic disease associated with structural damage to the joints. The pathological process is accompanied by degenerative deformation of the joint surfaces. In this case, not only cartilage tissue is damaged, but also bone tissue. The symptoms of the disease and its treatment depend on the extent of the joint damage.
The disease can develop for several years without showing any symptoms. At some point, under the influence of adverse factors (hypothermia, trauma, severe illness), the first signs of the disease appear. That is when it is necessary to consult a doctor, because the fight against dystrophic changes in the cartilage is especially effective at the onset of the disease.
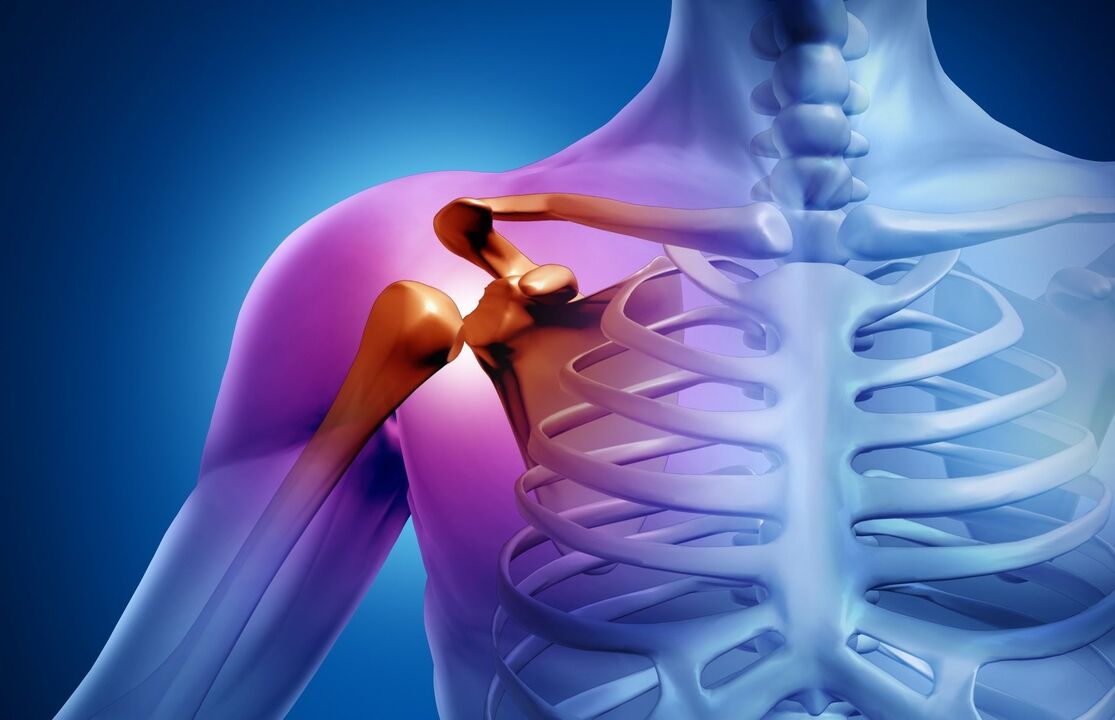
Causes of shoulder joint disease
The causes of degenerative-dystrophic damage to the tissues of the joints are many and varied. Among them, trauma plays a major role, therefore, post-traumatic shoulder osteoarthritis is considered the most common pathological form. It can be irritating even with mild, but repetitive damage to cartilage tissues.
In addition, the disease can occur under the influence of the following pathological factors:
- Severe joint damage: bursitis, gout, acute or chronic arthritis, aseptic necrosis of the vesicles.
- Frequent overwork of the joints. Often observed in athletes involved in volleyball, tennis, basketball.
- Congenital pathology of the shoulder joint.
- Endocrine diseases.
- Elderly and elderly people.
- Being overweight (obese).
- Avitaminosis.
- Autoimmune lesions and weakening of the immune system.
- genetic predisposition.
Most of the sick are monotonous manual workers. Therefore, arthropathy of the right shoulder joint is diagnosed much more often than on the left.
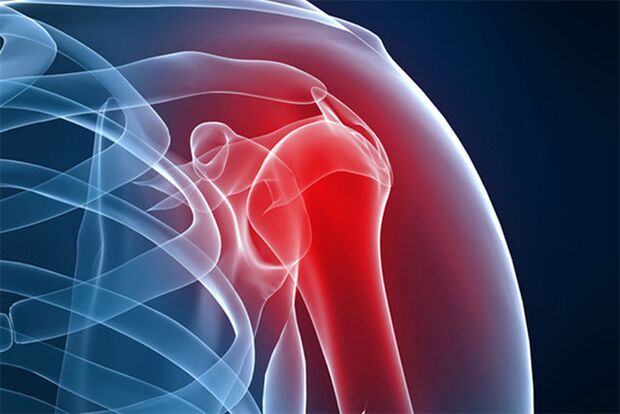
This disease often develops under the influence of not one, but several adverse factors at once. On this basis, the treatment must be comprehensive and aimed not only at combating the disease, but also eliminating all its causes.
Characteristic signs of the disease
The shoulder joint, which begins inconspicuously and gradually develops, can manifest suddenly after trauma, hypothermia, or severe exertion. In this case, there are characteristic symptoms of damage to the shoulder joint and adjacent tissues:
- pain;
- crunching and clicking when moving the hand;
- stiffness and reduced range of motion in the shoulder.
The disease usually occurs in a chronic form. An exacerbation of the disease can be triggered by excessive stress on the joint or an injury.
The intensity of symptoms is largely dependent on the severity of the cartilage and bone damage, so it is common to distinguish between degrees of disease. Such systematization greatly facilitates the diagnosis and allows you to accurately predict the outcome of the disease.
Shoulder arthritis grade I
During this stage, the tissues of the joint are mildly affected. Pain is observed extremely rarely and only after excessive physical exertion or prolonged monotonous work. Patients often do not pay attention to these symptoms, assuming they are caused by overwork or muscle tension. Lower than 1 degree is treated only with conservative methods.
In the early stages of the disease, on x-ray there are no obvious changes in the cartilage tissue, only an oval ring around the joint cavity is noted.
Shoulder arthritis grade II
At this stage, the symptoms of the disease become more pronounced. The cartilage tissue becomes thinner and deformed, the ligaments in the joint are damaged. During the movement of the hand will hear a crunching sound, the inner layer of the joint capsule is inflamed. Over time, the pain becomes constant. Stiffness and limited range of motion occur in the morning, which can lead to muscle atrophy.
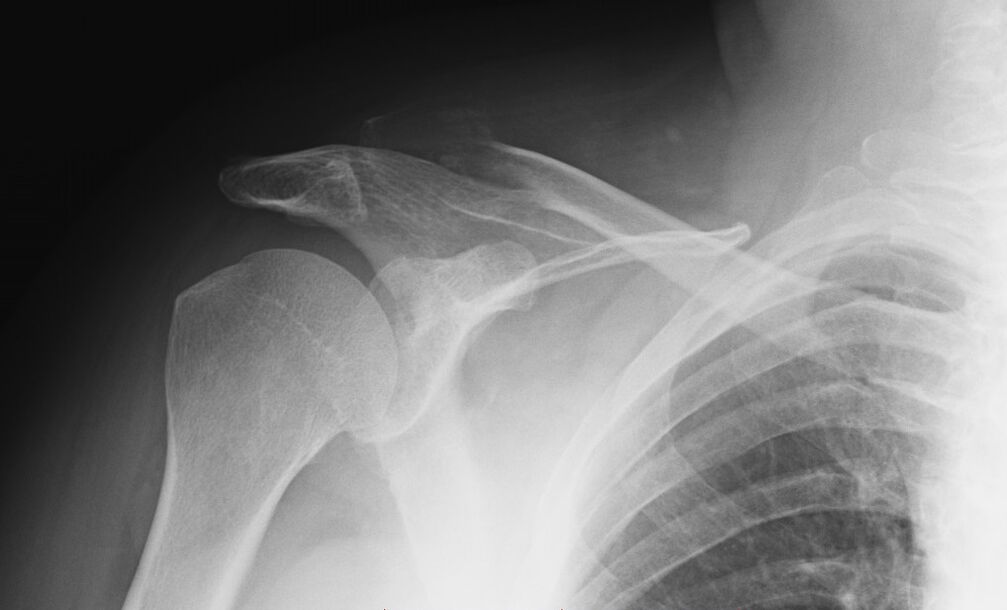
Shoulder arthritis grade III
During this period, the joint has become significantly deformed, there is almost no movement in it. The patient has acute pain that may radiate down the arm and shoulder blade. If you do not stop destroying tissues, the pathological process can lead to disability.
Grade 3 disease cannot be treated conservatively and requires surgical intervention.
Shoulder arthritis rarely reaches the third stage. Usually, the second stage is diagnosed as the transition to the chronic form.
Which doctor to contact?
Often, people dealing with joint pain don't know who to turn to. At the first symptoms of the disease, you should see a rheumatologist. The specialist will not only conduct a thorough physical examination and make a diagnosis, but also, if necessary, relieve severe pain with the help of an injection of anesthetic medication into the joint.
With the advanced form of the disease, the rheumatologist is potentially powerless. In this case, you will need to visit a surgeon or orthopedist. In large cities, you can make an appointment with a rheumatologist, who specializes only in diseases of the joints.
How to deal with shoulder arthritis
After examining and diagnosing the disease, the doctor will prescribe a specific therapy so that you can achieve long-term and stable remission of the disease. It is not possible to cure degenerative changes in the joints, but slowing down the destruction and alleviating the patient's condition is a perfectly feasible task.
The primary goals of antifibrotic therapy are to relieve pain and restore joint mobility.
Modern drug treatment
In some patients, it is difficult to make an accurate diagnosis in the early stages of the disease. At this stage, the pain is not obvious and does not force the patient to seek the help of specialists. Usually they are treated independently with folk remedies. Some patients engage in therapeutic exercises to relieve pain and stiffness. For the treatment of rheumatic diseases, drugs prescribed by a doctor are used, observing the recommended dosage and duration of administration. The most effective are the following groups of drugs:
- non-steroidal anti-inflammatory drugs;
- chondroprotectors;
- corticosteroid drugs;
- non-narcotic pain relievers;
- vasodilators;
- muscle relaxants.
Many drugs for this pathology are sometimes prescribed for a long time. Depending on the severity of the disease, the drugs are used orally, externally, intramuscularly or injected into the shoulder joint space.
Non-steroidal anti-inflammatory drugs (NSAIDs)
NSAIDs are contraindicated for long-term use due to their gastrointestinal side effects.
It is possible to treat the disease with drugs already in the early stages of the pathological development. The course of treatment is determined based on the patient's condition and severity of symptoms. As an independent treatment, ointments in this group are not prescribed. They are used in combination with similar classes of drugs that are administered intramuscularly or orally. Their task is to reduce inflammation and alleviate the patient's condition.
Chondroprotectors
Almost all patients are included in the treatment regimen with drugs aimed at improving metabolism in cartilage tissue. In addition, they also increase the elasticity of cartilage. Chondroprotectors have such properties. These medicinal substances differ depending on the main active ingredient on the basis of which they are made:
- hyaluronic acid;
- Chondroitin sulfate;
- glucosamine;
- combined funds.
Glucosamine is an important contributor to the formation of healthy cartilage tissue. The job of chondroitin sulfate is to nourish and cushion the shoulders.
Preparations for monotherapy are more proven on the market than combinations of many substances.
The polysaccharide contained in the intercellular space is hyaluronic acid. It may also decrease the sensitivity of receptors that respond to pain. Combined chondroprotectors, which contain several active ingredients, have the greatest advantage.
The use of chondroprotectors is most effective in the early stages of the disease. The task of the drug is to synthesize new cells of healthy cartilage tissue, replacing damaged tissue. When there is pain and swelling, drugs in this class are less effective. Therefore, it will be necessary to use anti-inflammatory drugs first to alleviate the patient's condition.
For maximum effect, injectable preparations are used for intra-articular or intramuscular injection. The course of treatment with chondroprotectors takes up to six months, some patients notice the first results after 3 months of treatment. It is important to follow some rules in the treatment of such drugs.
At the beginning of the course of treatment, physical overload, stress should be excluded. Patients will get the most benefit if they start taking chondroprotectors, improve their nutrition, and participate in physical therapy exercises. Many patients with osteoarthritis of the shoulder are carried out according to the method of Dr. Bubnovsky, they perform exercises specifically designed to achieve a gradual recovery of the joints or stop the progression of the disease.
Corticosteroid agents
When severe pain occurs, if anti-inflammatory drugs do not bring positive effects, people will prescribe corticosteroids. To alleviate the patient's condition, ointments or injections are prescribed.
Analgesic
In the early stages of the disease, analgesics are prescribed to relieve pain.
Compared with non-steroidal anti-inflammatory drugs, drugs of this class have less negative effects on the mucosa of the gastrointestinal tract.
Having an anti-inflammatory effect that has not yet been manifested, they effectively combat pain.
Vasodilators
Mandatory means in the treatment of rheumatic diseases are vasodilators. They eliminate spasm of blood vessels, normalize blood flow in the affected area. Many patients complain of the appearance of pain at night, which is effectively treated with drugs from this group.
Muscle relaxants
When you have shoulder osteoarthritis, muscle spasticity is considered a common phenomenon, this phenomenon will be relieved by muscle relaxants. When prescribing them, the principle of complexity is observed, they are used together with analgesics and anti-inflammatory drugs. If necessary, the minimum dosage is prescribed initially with gradual increments.
Surgical treatment
The main goal of surgery is to restore joint function and improve the patient's quality of life. If conservative treatment is ineffective, persistent pain syndrome persists, joint gradually deforms, markedly limited range of motion, the patient will be indicated for surgical intervention.
The decision about the need for surgery is made by the orthopedist or traumatologist together with the patient. Then the size of the endogenous and the material from which it will be made will be determined. Today, implants are made of titanium and high-strength polymers, and weigh nearly as much as a natural joint. The durability and reliability of endoprosthes is unquestionable.
Recovery time
The affected joint replacement operation is usually uncomplicated. Need to be fixed with a bandage for the first 14 days. Allows early passive performance of a combination of physical exercises on special equipment and devices. Electric load is allowed after 45-60 days.
Physical therapy
Any anti-arthritic complex exercise is helpful only when the disease is in remission. If there is an increase in temperature, aches and other symptoms of an exacerbation of the disease, then charging the battery is contraindicated.
Exercise therapy should not cause pain or discomfort. At the slightest inconvenience, exercise should be abandoned.

Battery charging should be done daily. After exercise, you should massage the affected joint and adjacent muscles yourself, using a healing cream that your attending physician will help you choose.
Physical therapy
Physiotherapy allows you to enhance the effect of the drug, reduce the dose and reduce the risk of complications. The type of physiotherapy is determined by the doctor, guided by the patient's condition, the neglect of the procedure and possible contraindications due to concomitant diseases.
Typically, the following physical therapy procedures are used in treatment:
- acupuncture therapy;
- ultrasound with hydrocortisone;
- electrophoresis with anti-inflammatory, analgesic agents;
- UV irradiation
- laser and infrared treatment.
Physiotherapy is carried out in courses of 10-15 sessions several times a year.
Treatment with folk methods
Combining folk remedies with drug treatment, exercise, proper nutrition and physical therapy, you can achieve long-term and stable remission of the disease.
One of the best recipes is a compress with birch leaves, which have anti-inflammatory and warming effects. Young leaves are most suitable, because the closer to autumn their beneficial properties decrease. Before applying, it is necessary to gently massage the affected limb. Then the leaves are applied to the skin, strengthened with cling film and bandages. Compression is left overnight. The duration of treatment is 10 days.
Salt baths have a healing effect. Before the procedure, the crystals are pre-dissolved in hot water. Then the resulting solution is poured into the bath. This process will require about 3 kg of salt. Alternatively, you can add a few drops of essential oils. It is best to take a bath before going to bed, bathing time should not exceed 30 minutes.
A hot compress with oatmeal helps a lot. They should be poured with boiling water, insisted and used for their intended purpose. Such procedures are recommended to be performed at night.
Many herbal poultices are useful. Crush the plants with anti-inflammatory effects (yester, ginger, turmeric, plantain, bovine jelly), boil with boiling water, close the lid for 10 minutes and then apply on the painful area. After the procedure, the affected shoulder should be put on a healing cream and go to bed.
Inside it is recommended to have an infusion of corn pistil. A teaspoon of raw materials or 1 filter bag is mixed with 200 ml of boiling water, covered for 30 minutes and consumed 1 tbsp. half an hour before meals.
Prevention of shoulder osteoarthritis.
Prevention can be primary and secondary. Primary prevention includes the following activities:
- regular exercise - jogging or brisk walking, exercises for the shoulder muscles;
- hot and cold shower;
- Eliminate excessive loads and avoid traumatic situations.
- timely treatment of diseases that can cause shoulder arthritis;
Secondary prevention aims at early diagnosis and treatment of arthritis.
Inference
Restoring joint function is a long and difficult process. Treatment of osteoarthritis of the shoulder should be primarily aimed at eliminating the symptoms of the disease. Only complex therapy, combining medicine and folk methods, can effectively relieve pain and restore working capacity.













































